
Gum recession (gingival recession) or receding gums refers to a condition where the gums move away from the crown of the tooth towards the roots, so that there is progressive loss of gum tissue, which eventually results in tooth root exposure if allowed to progress or left untreated.
Gum recession is not always easy to self-diagnose particularly in its earlier stages because the retraction of gums mostly takes place very slowly and usually without any symptoms.
Gum recession is a very common problem in adults but it may also occur starting from the age of a teenager and treatment almost always depends on the cause of gum recession.
The following symptoms are suggestive and common of gum recession:
When the gums recede far enough towards the roots so as to expose the cementum protecting the tooth root, the dentine tubules beneath will become more susceptible to external stimuli such as hot, cold, acidic and sweet foods and drinks. This gives rise to dentine hypersensitivity.
When gum recession is so severe that a large part of the roots of teeth become visible.
When gum recession is so severe so as to expose a large part of the roots of teeth, they appear to look much longer. As the gums continue to migrate towards the root end of the teeth, this can also result in “black triangles” Black triangles are large spaces between teeth as result of loss of gum tissue.
Plaque bacteria causes inflammation of gums which are more susceptible to bleeding. Inflamed gums are also tender which can lead to improper brushing and subsequently allows gingivitis or periodontitis to progress even further. Gum recession is common in patients who have severe periodontal disease so symptoms such as bad breath, inflamed and bleeding gums are usually indicative of gum recession or developing gum recession.
Improper use of an electric toothbrush or even scrubbing with a manual toothbrush known as traumatic tooth brushing can have a serious impact on the appearance of your gums.
Excessive force when brushing can start to wear away the gum tissue as well as the root surfaces creating notches or indentations within the roots of your teeth. Brushing too hard does not always ensure effective plaque removal or good oral hygiene.
Gum disease is caused by plaque bacteria that is allowed to accumulate on the teeth and gums, resulting in inflammation of gums and the destruction of periodontal ligaments, and bone that holds the teeth in place within the jaw bone.
As periodontal disease is allowed to progress, this then leads to gum recession. However, if you have poor oral hygiene and swollen and inflamed gums, you may not always notice the extent of gum recession until your oral hygiene improves.
Once meticulous self-performed oral hygiene is carried out to include cleaning in between teeth and following appropriate periodontal treatment, the inflammation, swelling and bleeding will gradually begin to reduce, revealing the true extent of gum recession.
This is caused by active (untreated) periodontal disease and not as a result of the treatment or improved oral hygiene. This is why it is so important to ensure that meticulous self-performed oral hygiene is always maintained to prevent inflammation of the gums starting in the first place.
The more severe the gum disease, the more gum recession will be noted. Other causes of periodontal disease include systemic conditions such as uncontrolled diabetes and smoking.
Oral piercings of the tongue, lips or cheek can cause localized gum recession. Patients who have had tongue piercings are more likely to develop gum recession in the lower lingual (near, or on the side towards the tongue) region of their anterior (front) teeth than patients without any piercings.
Gum recession can increase the risk of sensitivity as it wears off the enamel of your teeth resulting in poor aesthetics. Other complications of piercings include: tooth fracture, abrasion of teeth (excessive wear), speech impediment, infections and allergic response.
It is the biggest cause of periodontal disease and causes the destruction of the gums, periodontal ligaments, and bone that holds the teeth within the jaw bone and contributes to gum recession in the same way as active or untreated periodontal disease.
Smokers tend to have a reduced response to non-surgical and surgical intervention or treatment and are at a much higher risk of developing infections. Smokers tend to build more tartar deposits on their teeth and have more gum recession than non-smokers.
Previous orthodontic treatment may contribute to gum recession. The lower central incisors and the upper first molar teeth are the most commonly affected.
Movement of teeth outside the jawbone has been shown as a risk factor for gum recession. A combination of a previous history of orthodontics where the roots of teeth have been moved outside the jawbone to facilitate correct tooth position and poor oral hygiene leading to inflamed and bleeding gums can exacerbate gum recession
If your teeth are not in alignment to one another, gum recession can occur in this situation due to the roots of the teeth not being well centered within the jawbone.
Every case of gum recession is different; however the root cause of the gum recession must be identified and addressed for the best possible gum disease treatment outcome. Usually your Specialist Periodontist will help you identify the cause and will instruct you on how to minimize gum recession.
If overly aggressive brushing techniques or traumatic (overzealous) toothbrushing is the cause of your gum recession, re-evaluating your brushing habits by using a medium textured toothbrush or correct brushing technique may be recommended to minimise the problem.
If poor oral hygiene is a problem and has lead to gingivitis (inflammation of the gums), professional dental cleaning may be recommended to remove tartar and plaque bacteria from within the gum pockets.
In the case of severe periodontal disease (inflamed gums with the progressive loss of bone), professional mechanical plaque removal under local anesthetic is usually performed to achieve periodontal health.
Many patients dislike the aesthetic effects of recession, such as longer looking teeth and the “black triangles” that appear in-between, however depending on the cause of your gum recession, your Specialist Periodontist or gum specialist may recommend surgical treatment to improve aesthetics.
A gum graft (also known as a gingival graft or periodontal plastic surgery) is a collective name for surgical periodontal procedures that aim to cover an exposed tooth root surface with grafted tissue from the roof of the mouth (palate).
The main purpose of gum grafting is to create an adequate zone (width) of attached gum tissue so as to facilitate oral hygiene and prevent the likelihood of further gum recession. It is an excellent way to restore the natural symmetry to the gums and make the smile look more aesthetically pleasing as well as to increase the thickness of gum tissue.
Thicker gums are more resilient to further gum recession or relapse following gum-grafting procedures. This procedure is usually done by your specialist periodontist.
Here are some of the most common types of gum grafting:
This procedure is often used to create a wider zone of attached gum. A layer of tissue, the epithelium and connective tissue is removed from the palate and grafted to the area affected by gum recession.
Both surgical areas where the tissue has been removed from usually the palate (roof of mouth) and the grafted site (area of recession) will quickly heal uneventfully, however following healing, the grafted site is usually slightly paler in color that the surrounding gums due to the graft which has intact epithelium.
This procedure is commonly used to thicken gum tissue and to cover exposed roots to provide root coverage. Here the epithelium is eliminated and only the connective tissue from the roof of the mouth is harvested and grafted to the area of recession. This results in optimal aesthetics
This procedure uses medically processed, donated human tissue as a tissue source for the graft. The advantage of this procedure is that there is no need for a donor site surgery from the patient’s palate (and thus, less pain).
Gum grafting is a common periodontal procedure carried out by Specialist Periodontist and can result in excellent aesthetics and increase the long-term prognosis of teeth affected by gum recession.
Here are some of the major benefits associated with gum grafting:
When the tooth root becomes exposed, eating or drinking hot or cold foods or even acidic and sweet can cause extreme sensitivity to the teeth. Gum grafting surgery permanently covers the exposed root, helps reduce sensitivity, and restores aesthetics.
Periodontal disease is characterized by gum recession, inflammation and bone loss. Gum recession and root exposure can make the teeth look longer than normal.
Gum grafting can make the teeth look shorter, more symmetrical and generally more pleasing from an aesthetic point of view.
However it is important to note that where there has been extensive underlying bone loss, particularly in between teeth as a result of periodontal disease, gum-grafting procedures are unsuccessful and will not provide root coverage. For gum grafts to be successful, adequate bone levels must be evident.
Periodontal disease can progress and destroy gum tissue very rapidly. If left untreated, a large amount of attached gum tissue can be lost in a short period of time.
Toothbrushing can then become painful, especially where there is a lack of attached gum tissue. Pain will then result in inadequate brushing and will allow continued inflammation which will then continue to progress unless brushing is improved.
Gum grafts can facilitate oral hygiene by providing a wider band of attached gum tissue making brushing pain free.
Your Specialist Periodontist will inform you whether a gum graft will improve the long –term prognosis of your tooth.
In some cases where there has been advanced gum recession, no surgical intervention can result in progressive gum recession and possible future risk of tooth loss.
However your Specialist Periodontist may advise you to consider a gum graft procedure in order to prevent progressive loss of gum tissue and to increase the long term prognosis of your teeth affected by recession
Once the need for gum grafting surgery has been determined, there are several treatments your Specialist Periodontist will want perform before gum grafting can take place.
First, the teeth must be thoroughly cleaned supragingival (above the gum margin) and subgingivally (below the gum margin) to remove calculus (tartar) and bacteria. This will eliminate any inflammation and reduce the tendency of your gums to bleed, making subsequent surgical procedures easier to perform.
The gum grafting procedure is usually performed under local anaesthetic. The exact procedure will depend much on whether tissue is coming from your palate (roof of the mouth) or a tissue bank (donor).
Initially, the recipient site is prepared by making small incisions in the area where the graft will be placed. Then another incision is made in the roof of your mouth (donor site) to harvest the connective tissue graft, which is then grafted onto the recipient bed.
Stitches are first placed to close the area where the graft has been harvested from and then stitches are used to secure the graft to the recipient bed. Uniformity and healing of the gums will be achieved in approximately 3-4 months following the surgical procedure.
Treatment options and outcomes depend highly on individual cases
While this could be considered a low risk procedure, risks related to connective tissue grafting might include, but are not limited to, post-operative bleeding, pain, swelling, soreness, numbness, infection, facial discolouration, bruising, transient or, on occasion, permanent tooth sensitivity to hot, cold, sweets or acidic foods, failure of the procedure / graft and increased recessionof the affected tooth and temporary numbness of the donor site – palate (roof of the mouth), bigger spaces between teeth and food impaction.
Below are some pictures following surgical gum grafting procedures using both tissue from the patient’s palate (roof of the mouth) or a tissue bank (donor).

Root coverage using connective tissue harvested from the roof of the mouth.
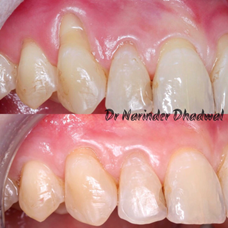
Root coverage using Acellular Dermal Matrix Allograft
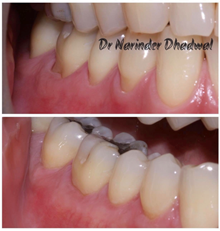
Root coverage using Acellular Dermal Matrix Allograft
If you have any questions about soft tissue grafting, please ask your Specialist Periodontist, dentist or hygienist.
ADDRESS: 94 HARLEY STREET, LONDON, W1G 7HX
TEL: 020 7580 4200 | SMILE@SPECIALISTDENTALSERVICES.COM
Fields with (*) are required.
Please contact us via this website or email without disclosing confidential information.


